Endoscopes are medical devices designed to collect the smallest images from inside the human body. Endoscopes can be divided into two categories: rigid endoscopes, in which relay lenses are stacked together generally creating a high-quality image, and flexible ones-devices of lower cost where a camera is inserted near the tip of the endoscope while the image is transmitted via wires or fiber optics. In today’s articles, we will talk about the design parameters of a rigid endoscope. In a future blog entry, we will discuss the design of flexible endoscopes.
Components
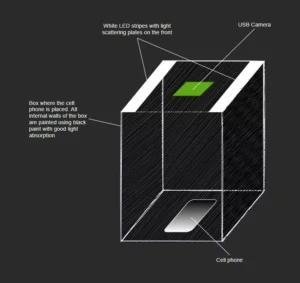
There are some basic components of any endoscopic system. First, we need a light source. Traditionally, xenon sources are used (and less commonly, metal halide and tungsten halogen). In recent years, LED broadband LED sources are becoming more common. The second thing needed is a way to transfer the light inside the human body. Usually, a ring of optical fiber is used for this task.
It is important to note that the illumination light doesn’t go through the optical lenses used to observe the surgery. Endoscopes use the light that is tissue-scattered to create the image to avoid the final image degradation from the back light reflection in the optical system.
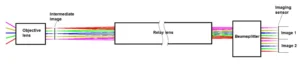
Traditionally, rigid endoscopes use relay lenses to relay the image from an objective lens to the camera sensor. In a past article, we talked about the fundamentals of relay lenses where we talked about a borescope which has a design very similar to a rigid endoscope. A schematic of a rigid lens can be seen in Figure 1.
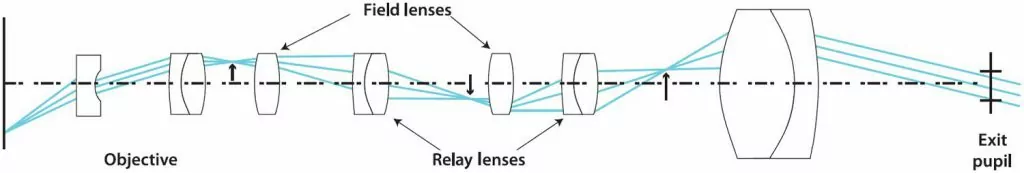
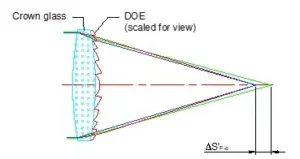
It is possible to substitute some of these relay lenses by Gradient Refractive Index lenses (GRIN). The main advantage of GRIN lenses is that they simplify the manufacture of endoscopes. A drawback however is the reduction of field-of-view and a diminished brightness due to the low GRIN lenses numerical aperture.
Endoscope Specification
As with any medical instrumentation, there are very strict controls on endoscope designs from their length and diameter, to the field of view and image resolution. However, some aberrations that may be important in an industrial setting are less important here. For example, distortion is well accepted due to the wide-angle view needed.
Sometimes the surgeon needs to observe a portion of the body not directly in front of the endoscope tip. In the case of knee surgery using endoscopes (arthroscopes), it is sometimes necessary to observe at a direction of 30 to 70-degrees. So it is necessary to attach prisms to the endoscope tip.
In case of physical dimensions, the diameter is a very important parameter. A typical knee arthroscope has a shaft diameter of 4-mm. Contained in that diameter we have an outer tube, a smaller tube that contains the illumination systems, and a third tube that contains the relay lenses. This limits the size of the optical components to around 2.8 mm in diameter.
The lens diameter sets the limit of almost every other parameter. The lens diameter limits the lens f-number and therefore the image brightness. Even if there is a need for higher illumination, there is a restriction on the number of optical fibers that can be added in the remaining space.
The ISO8600 standard is used to evaluate the endoscope performance. This is an old standard but it is still useful and can help set up a basic framework to develop our designs.
There is a lot more information about the design of endoscopes and a single article won’t be enough to cover all possible topics. If you are interested in learning more, I’ll recommend D. Leiner’s book “Digital Endoscope Design” as a good introduction to this topic.